Caregiver Burnout: When Caregiving Becomes a Battle.
- Joanna Szczeskiewicz

- 1 day ago
- 8 min read

Caring for another human being while trying to maintain a life of your own is not a "journey." It’s a grind. Whether it’s a disabled child, aging parents, or a partner with a chronic illness, the reality is the same: the demands are endless, the stakes feel lethal, and the quiet moments are terrifying because that’s when your brain finally has time to panic. It’s not just fatigue. It’s a permanent state of bracing for impact. You are vibrating with a frequency of "readiness" that never actually turns off.
Most advice tells you to get organized or "find time for yourself." That’s useless when relaxation feels dangerous or just wrong. Let's look caregiving stress through the lens of Process-Based CBT (Cognitive-Behavioral Therapy). We aren’t going to talk about "thinking positive." We’re going to talk the Cognitive Attentional Syndrome (CAS)—and how it keeps you trapped in emergency mode even when you do not need to be. Emergencies do happen but we do not have to be on a constant lookout. So, even when everyday pressures feel relentless—like being encircled by wolves, unable to pause for fear that something will go wrong at any moment—developing the ability to distinguish between real danger and pressure can make us more effective, allow for moments of rest, and open up space for genuine human connection.
Three Versions of the Same Trap
Let’s look at three people who look different on paper but very similar inside of their heads.
Maya: The Project Manager Maya is 39. She runs a high-stakes medical unit by night for her 10-year-old son, Eli. Her alarm goes off at 5:30 a.m. to lift, feed, and medicate. By the time she logs into her actual job at 8:30 a.m., she’s done a day’s worth of labor. But the real drain happens at 9:00 p.m. Eli is asleep. The house is quiet. Maya sits on the sofa, body throbbing, but her mind is accelerating. “Did I miss a line on that insurance appeal?” “His breathing sounds wet. Is that pneumonia?” She scrolls forums looking for reassurance and finds horror stories instead. She is technically "off duty," but her nervous system is sprinting.
Carlos: The Sentinel Carlos, 52, is the sole support for his mother, Rosa, who has dementia. His day is a blur of work and pharmacy runs. But his torture is the hypervigilance. Every time his phone buzzes, his stomach drops. At night, he stares at the ceiling. “If I let my guard down, she’ll fall.” “I shouldn't be angry. I’m a terrible son for feeling this heavy.” He believes his worry is the only thing keeping her safe.
Aisha: The Anchor Aisha is 60. She supports her 88-year-old father and two adult children who can’t seem to launch. She is the bank, the therapist, and the driver. Her internal monologue is a list of other people's needs. “I’ll relax when Dad’s appointment is done. No, when the roof is fixed.” The horizon of "done" keeps moving. Even when she sits to watch TV, she is only half-there, hijacked by a retrospective of her past mistakes.
Cognitive Attentional Syndrome (CAS)
Process-Based CBT focuses on how you think, not just what you think. Maya, Carlos, and Aisha are stuck in CAS. It consists of three habits:
Worry: Repetitive "What if?" thinking about the future.
Rumination: Repetitive "Why?" thinking about the past.
Threat Monitoring: Constantly scanning for danger or failure.
Your brain loves CAS because it feels productive. It feels like problem-solving. If I worry enough about the form, surely I won't miss a mistake. But CAS is a trap. It keeps your nervous system in "Fight or Flight" regardless of what is actually happening. It effectively tells your brain: “Do not stand down. The predator is still here.”
The Wolf Test
Your nervous system evolved to handle predators (wolves). When you see a wolf, your cortisol spikes, your focus narrows, and you stop digesting food. You survive the next ten minutes.
Caregiving triggers this same biology. But here is the distinction: Most caregiving moments are high in burden, but low in danger.
The laundry is piled up? Burden.
Your parent is repeating the same question? Burden.
You are arguing with insurance? Burden.
Are you currently under physical attack? Here is the "Wolf Test": If you were truly surrounded by a pack of wolves, could you safely close your eyes for 60 seconds? Could you hold a cup of coffee? Could you take a slow breath without being mauled?
If the answer is "Yes, I can physically do those things," then you are not facing wolves. You are facing tasks.
This matters because you cannot reason with a nervous system that thinks it’s being hunted. You have to show it that it is safe. When you treat tasks like wolves, you burn out because you never recover.
Why You Can’t Relax
CAS insists: “It is not safe to switch off.”
Carlos lies in bed while his mother is asleep. The house is locked. The danger is effectively zero. But his CAS says, “If you relax, you are irresponsible.”
You need to catch this mechanism in real-time. Say to yourself: “My mind is in CAS mode. It’s replaying conversations and predicting disasters. That is a habit, not a reflection of reality.”
Worrying is Not Doing
We cling to CAS because we confuse mental churning with action.
Worry feels like planning. But planning leads to an action (calling the doctor). Worry just circles the drain.
Resentment feels like justice. But fuming about your sister doesn't change her behavior; it just burns your energy.
Hypervigilance feels like focus. But staring at a sleeping child for two hours doesn't make them safer; it just makes you sleep-deprived.
Ask yourself: “Is what I am doing with my brain right now moving a task forward? Or am I just revving the engine in neutral?”
Guilt and Realism
Caregiving breeds "Moral Residue"—that nagging feeling that you aren't doing enough. This usually comes from confusing two types of responsibility:
Causal Responsibility: Who caused the illness or aging? (Nature, genetics, bad luck. Not you.)
Remedial Responsibility: Who is trying to fix it? (You.)
You are carrying the remedial load with the weight of causal guilt. You act like you broke the vase, when you are just the one trying to glue it back together. In this context acceptance isn't passivity but factual realism. “This is the situation. It sucks. I did not cause it. I cannot fix it entirely. I can only influence certain variables.”
Practical Shift 1: The Body
You cannot talk your body out of stress. You have to behave your way out of it. You need to give your nervous system evidence that the wolves aren't there.
The Micro-Pause If you were fighting a wolf, you wouldn't close your eyes. So, closing your eyes for 60 seconds is a signal to the brain that you are safe. Sit down. Close your eyes. Drop your shoulders. Breathe.
The Progressive Release Tense your hands into fists for 5 seconds. Squeeze hard. Then, let go. You are teaching your body the difference between "braced" and "soft."
These aren't relaxation hacks. They are biological signals. They tell the brain: “We are safe.”
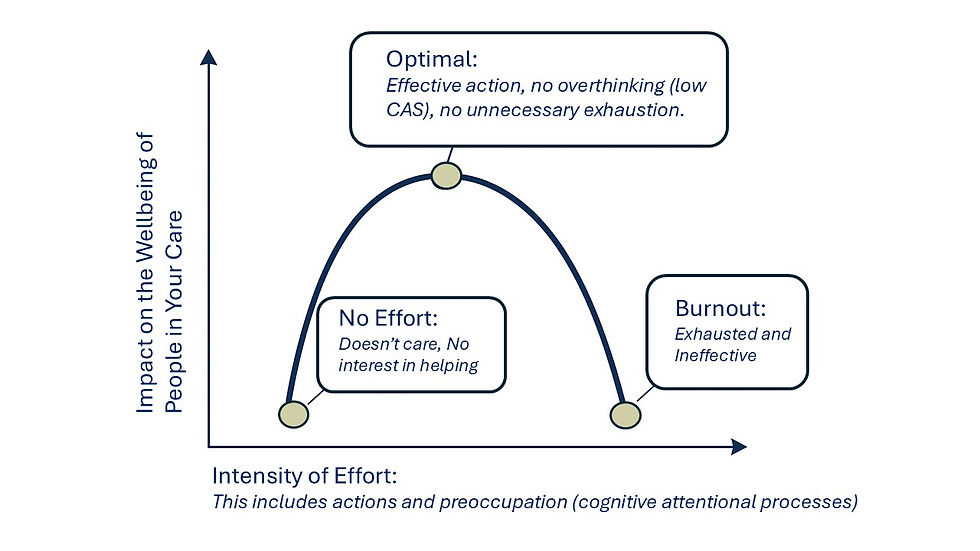
Practical Shift 2: The Inverted U
There is a belief in caregiving that harder is always better.
Picture an inverted "U" shape. On the left, as effort increases, your impact increases. You organize meds, you cook, you drive. This is the sweet spot. But there is a peak. Once you cross that peak—into the zone of no sleep and obsessive checking—your effort goes up, but your impact goes down.
You become irritable. You make errors. You injure your back. White-knuckling the steering wheel doesn't make the car drive straighter. It just exhausts your arms. Ask yourself: “Where am I on the inverted U? Have I passed the peak where my extra effort is actually making things worse?”
Practical Shift 3: Intentionality
Caregivers often feel stripped of choice. “I don’t have a choice, they need me.”
You can't choose the diagnosis, but you can choose the micro-moments.
“I am choosing to wash these dishes now so the kitchen is clean.” (Vs. “I have to do this.”)
“I am choosing to watch this show and put my phone in the other room.”
This requires attention training. CAS smears mud on your mental windshield. Attention training wipes it clean. When you drink coffee and your mind runs to the future, pull it back. “Not now. I am drinking coffee.” You might have to do this 50 times in one minute. That’s the rep. You’re building the muscle to be present.
The Venn Diagram of Reality
To target guilt, let's visualize three overlapping circles. The circles are not the same size and don't quite overlap like a typical Venn diagram (see below).

Let's look at it again:
Needs: What does your loved one truly need for safety and dignity? (Food, hygiene, meds).
Aspirations: What do you wish you could give them? (A cure, total happiness, a perfect life).
Resources: What do you actually have? (Money, energy, time, the medical system).
Suffering lives in the gap between aspirations and resources. We beat ourselves up for not providing the aspirations, even when our resources make it impossible.
Focus on the overlap between needs and resources. If you are meeting the needs with your available resources, you are succeeding. Letting go of the aspirations that don't fit is not failure. It is a necessity.
The "Special Project" Trap
When the pain of a loved one's decline is too much, we often detach and go into "fix-it" mode. We obsess over metrics and schedules. We become their case manager, but we stop being their partner or parent. Heck, many caregivers guilt-trip themselves:
“How can I go out when they are suffering.” (Your having little fun is not going to make their condition worse.)
“A good mother sacrifices everything.” (What if that mother is so exhausted that she is no longer able to mother?)
If you treat yourself like a disposable resource, you will eventually be disposed of—by burnout or illness.
Treating a loved one as a "special project" dehumanizes them. It reduces them to a problem to be solved. Sometimes, care is stopping the "fixing" for an hour and just sitting with them, letting the problem exist, unsolved.
A Two-Pronged Approach
So, how do we stop our responsibilities from turning into wolves?
1. Participate Fully in What Is. Stop waiting for the "caregiving phase" to end. This is your life. It is heavy, but it also contains your morning coffee and the feeling of clean sheets. Use your attention to actually be there for the non-caregiving moments. When you are off duty, be off duty.
2. "Office Hours" for Optimization. We all want to improve things. But letting that search consume every waking hour is CAS. Set "Office Hours" for research.
“On Tuesdays from 7 p.m. to 8 p.m., I will research treatments and think about the future.” When the thought comes up on Wednesday morning, note it: “I’ll handle that during Office Hours.”
This keeps the "fixing" in a cage so it doesn't run wild through your life.
You Are Still Standing
As caregivers we might hate the situation we are in. That is valid. We can acknowledge that the hand we’ve been dealt is not our first choice. Look at yourself. You are still standing. You are managing a level of complexity that would crush most people. You are doing it with grit.
You are not a bad person for needing to sleep. You are not a failure for taking a break. You are not cold for refusing to let worry burn your mind down.
The wolves are a biological error. The tasks are real. And so is your love. You are fully capable of handling the tasks, as long as you stop fighting the wolves. That is how you reclaim the bandwidth to not just care for your loved one, but to actually feel the affection that nourishes you both.




